Frailty isn’t defined by age alone. Compared with other patients the same age, frail people are at greater risk of adverse health outcomes, like death. Therefore, it is vital that frailty is measured easily and objectively and identified early in their care journey. Frailty screening can help identify those vulnerable older patients who require customised care. A more comprehensive assessment will then be completed where frailty is determined.
The Frail Older Persons Collaborative defined 'frailty' as a state of increased vulnerability, associated with but distinct from increasing age and multi-morbidity, resulting in disproportionate adverse health outcomes following a stressor, which has been endorsed for use across Queensland Health.
Initiatives
The Clinical Frailty Scale (CFS)—developed by Professor Kenneth Rockwood—has been endorsed as the agreed standard frailty screening tool across Queensland. It can predict adverse outcomes in older people in hospital, including hospital-based harm, ED and inpatient length of stay, the need for aged care facility placement, and even death.
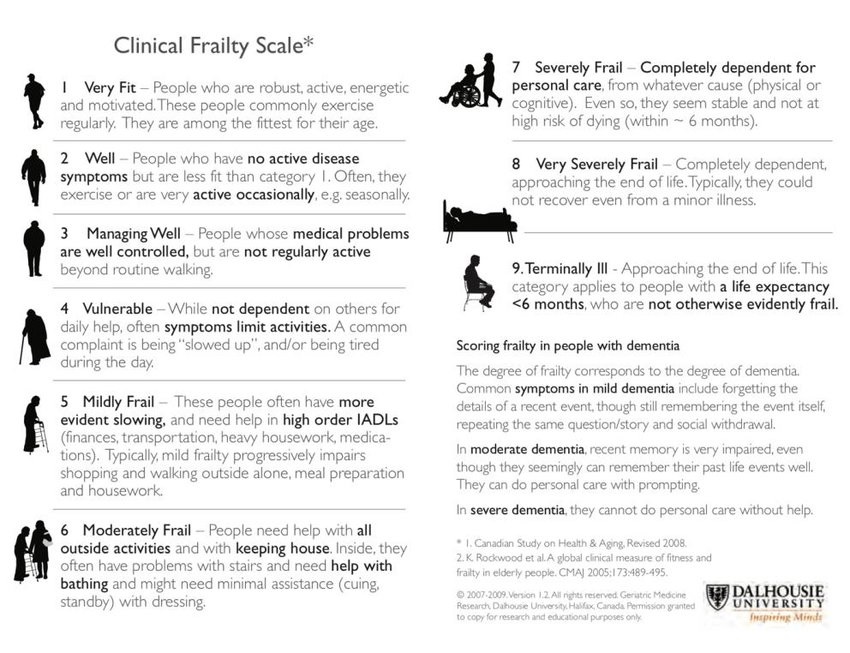
ED clinicians can use the tool to quickly recognise and quantify frailty through clinical judgement to inform their practice. The CFS can also be used as a prioritisation tool for patient flow. For example, patients scoring between 1-3 on the CFS are considered fit and healthy and able to be moved through the usual care path, versus patients 4-9 who are likely to need more help.