A unique Queensland first, nurse-led vascular access team is reducing catheter-associated complications and improving the patient experience.
Sunshine Coast Hospital and Health Service’s vascular access surveillance and education (VASE) service sees specially trained nurses insert peripherally inserted central catheters (PICCs), guided by ultrasound.
The service started in 2009 with bedside insertion (confirmed by chest x-ray), and expanded to use the ECG method in February 2016, negating the need for a chest x-ray. The team currently performs around 1,600 PICCs per year.
PICCs are specialised catheters that can provide reliable venous access. The use of PICCs has risen significantly over the past 35 years, particularly given the many advantages of the device and the lower complication rates when compared with traditional central venous catheters (CVC).
The insertion of a PICC means patient care can be continued in a non-inpatient setting such as Hospital in the Home and outpatient clinics, which helps improve bed utilisation and patient flow.
Leanne Ruegg, Clinical Nurse Consultant with the VASE service said historically, PICCs were inserted by a medical officer. “The first nurse-led vascular access team was established in the United States in the 1970s,” she said.
On the Sunshine Coast, PICCs are confirmed by using the Sherlock 3CG®tip system which has a sensor that tracks a magnetic tip relative to the heart and placed at the Cavo-atrial junction.
Leanne said the team recently conducted a retrospective analysis of 661 PICC insertions. The study, Peripherally inserted central catheter-associated complications: a retrospective review of a nurse-led peripherally inserted central catheter-insertion service, found the nurse-led service demonstrated minimal infection and thrombus complications.
“We reported lower rates of catheter-related bloodstream infections and catheter-related deep venous thrombosis than other previously published studies.”
Leanne attributed the low complication rate to the highly experienced nurses in the team, the use of a standardised insertion bundle, and the tip navigation/confirmation system.
“The results are reassuring and a clear indication of the benefits of nurses working to top of scope. The VASE team continues to insert the majority of PICCs,” Leanne said.
In addition to reduced complication rates, the innovative model also decreased the time patients had to wait for a PICC insertion and reduced costs by minimising the use of interventional radiology suites.
“This model is very cost effective, mobile, more efficient, means the patient doesn’t have to be exposed to radiation, and can be used immediately,” Leanne said.
“The benefits are clear, and it means medical and IR staff can spend more time on more complex patients,” Leanne said.
She advised other sites looking to implement the model to consider organisational culture.
“The concept of a nurse-led service clearing PICC lines requires a cultural change. The support from clinical and senior medical staff played a significant role in our success.”
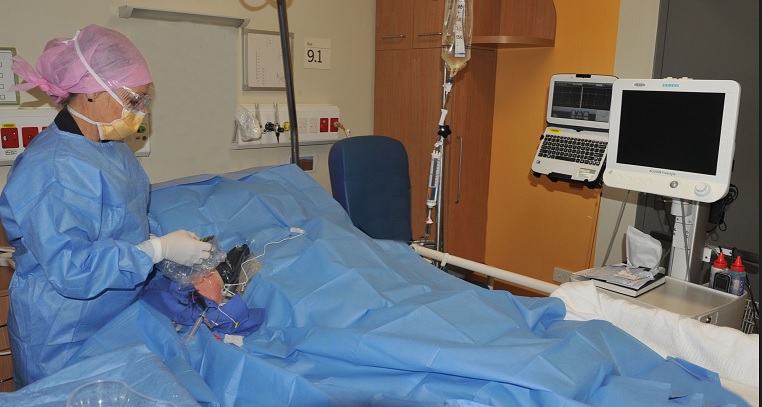
Leanne Ruegg, Clinical Nurse Consultant, performs a peripherally inserted central catheter on a patient